Neuropathic pain: when something gets on your nerve
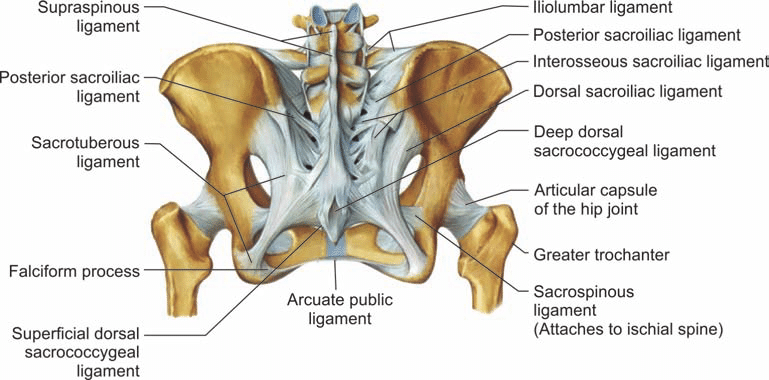
I recently had a podiatrist send me a patient. The podiatrist told the patient their foot pain was coming from their spine rather than their feet. I was impressed that the podiatrist understood the connection between pain in the feet and the spine. He had correctly determined that the patient’s pain was neurogenic or neuropathic, due to either dysfunction or damage of the nervous system as it passes through the spine, rather than trauma, dysfunction, or disease of the of the muscles, ligaments, joints or bones of the feet.
Sciatica, leg pain, from a pinched nerve in the low back due to a herniated disc is a neuropathy that we commonly treat. Neuropathic pain can be experienced as:
- Spontaneous pain (pain that comes without stimulation):
- Shooting, burning, stabbing, or an electric shock-like pain;
- Tingling, numbness, weakness, or a “pins and needles” feeling.
Untreated it can progress through 5 stages:
- Occasional numbness and pain,
- More regular symptoms,
- The pain reaches its high point,
- Constant numbness, and
- A total loss of feeling.
The neuropathic symptoms of may improve or be cured if the underlying condition causing the neuropathy is cured or better managed. The real key to resolving neuropathic pain is addressing its cause in the early stages, before it becomes more constant or increases in intensity.
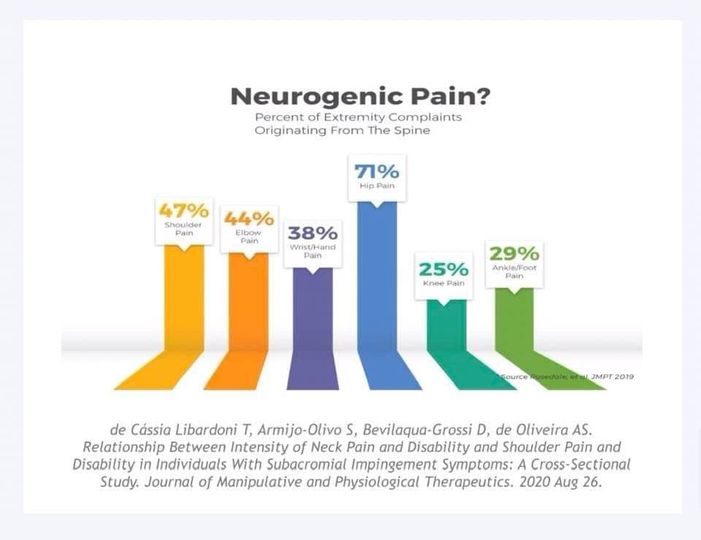
While as many as 10 percent of Americans experience some form of neuropathic pain is not normal. The experience of pain means that something is wrong and the pain should not be ignored. Neuropathic pain experienced in the extremities commonly originates in the spine. There is a:
- 47% chance that shoulder pain originates in the spine rather than the shoulder,
- 44% chance that elbow pain originates in the spine rather than the elbow,
- 38% chance that wrist/hand pain originates in spine rather than the hand or wrist,
- 71% chance that hip pain originates in the spine rather than the hip,
- 25% chance knee pain originates in the spine rather than the knee and a
- 29% chance that ankle/foot pain originates in the spine rather than the foot or ankle.
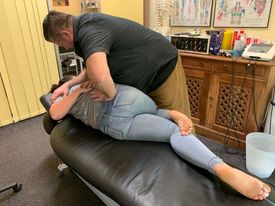
If extremity pain does not resolve with exercise or therapies applied directly to the extremity there is a high probability you are dealing with neurogenic pain. Addressing the cause of the pain, the spine, during the early stages of of the condition with chiropractic care, decompression traction and regular exercise are three keys to resolving extremity neuropathic pain. Delaying treatment could lead to chronic pain and a total loss of feeling, leaving the patient with no option other than drugs, surgery or trying to live with severe chronic pain. Over time, neuropathic pain can lead to serious disability and complications, including depression, problems sleeping, anxiety, and more. We have a good track record for treating spine related neuropathic pain in the extremities. Give us a call and make an appointment.



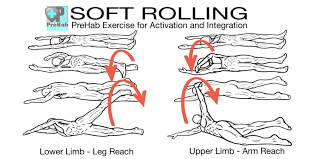
 While lying on your stomach may feel great, like getting a full body hug for as long as you want, it’s not good for your neck and can contribute to more than a poor night’s sleep. If you wake up irritable with neck pain, headaches or tingling in your fingers, keep reading.
While lying on your stomach may feel great, like getting a full body hug for as long as you want, it’s not good for your neck and can contribute to more than a poor night’s sleep. If you wake up irritable with neck pain, headaches or tingling in your fingers, keep reading. When to take the tape off in the morning you have a stiff and sore finger. You would not do that to a normal healthy finger so why would you do that to your neck?
When to take the tape off in the morning you have a stiff and sore finger. You would not do that to a normal healthy finger so why would you do that to your neck?






Peak performance: abnormal forward head posture impedes sports performance
August 21, 2022 by manager • Uncategorized
Postural pain syndromes and headaches, caused by forward head posture, are common but not normal. Headaches and neck pain are just the tip of the iceberg. Abnormal forward head posture (FHP) is also correlated with diminished balance, speed and strength.
A recent study published in the Journal of Sport Rehab evaluated skill-related differences in physical fitness between two groups of pain-free college athletes that played volleyball, handball or basketball. 50 athletes with abnormal (FHP) were strictly matched with 50 controls with normal head posture.
Abnormal FHP was defined as having a craniovertebral angle (CVA) less than 55°. The craniovertebral angle, A, in the photo is calculated by:
Abnormal forward head posture stretches the spinal cord, putting it under tension, reducing the speed of nerve impulse velocity in the spinal cord by 10 – 20 %.
All the athletes completed four physical fitness skills test: (1) T- test (agility and speed), (2) stork (static balance) test, (3) Y-balance test (dynamic balance) and (4) vertical leap (leg power) and the results of the two groups were compared.
T – test Stork test Y – Balance vertical leap
Conclusion: College athletes with FHP of less than 55° exhibited less efficient skill-related physical fitness when compared with athletes with normal sagittal head posture. On average athletes with abnormal FHP were 1 second slower in their agility sprint times, their vertical leap was 9 cm lower, their ability hold the stork balance test was several seconds less and their dynamic balance was poorer than athletes with normal head posture.
A FHP of 55° or less on a photograph correlates with an anterior head translation of 25mm or more as measured on x-ray, which is a more accurate and our preferred way of measuring abnormal FHP . A CVA closer to 90 degrees = 0mm of anterior head translation. There is a linear relationship between the magnitude of FHP and speed, balance and power in healthy pain free athletes. Better posture = better fitness skills outcomes. Other posture studies have shown that bodies heal faster and stronger when their spinal cords are not under tension. Another study showed ocular motor control reaction time, the ability to track an object in space, is slowed with abnormal FHP.
At Doctors of Chiropractic Capalaba we are not limited to treating pain. We can change posture, spinal cord tension and spinal cord nerve impulse velocity which improves sensory processing, speed, balance and power. Correcting and maintaining good posture and spinal mobility is an essential part of health and wellness. You do not have to be an athlete to experience the benefits.
Reference: Journal of Sport Rehab: Comparison of Sensorimotor Integration and Skill-Related Physical Fitness Components Between College Athletes With and Without Forward Head Posture, By Drs. Ibrahim Moustafa, Meeyoung Kim, Deed E. Harrison